Risks from radiological & nuclear medicine examinations
 The basis of present day medicine is shared decision making between the doctor and the patient. Empowering a patient to make informed decisions about their treatment is a fundamental principle in medical professionalism. But is this principle translated into clinical practice in so far as radiological and nuclear medicine examinations are concerned?
The basis of present day medicine is shared decision making between the doctor and the patient. Empowering a patient to make informed decisions about their treatment is a fundamental principle in medical professionalism. But is this principle translated into clinical practice in so far as radiological and nuclear medicine examinations are concerned?
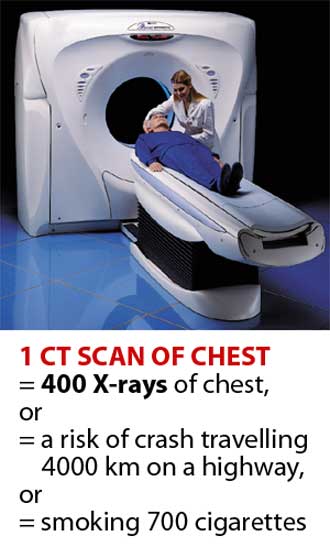
In general, patients undergoing radiological and nuclear examinations receive no, very little, or inaccurate information regarding the risks involved. Take, for example, the CT Scans and X-rays. They are so common that they are used as if they don’t pose any risk.
As every examination of a radiological or nuclear medicine nature involves the administration of radiation, there is the inherent long-term risk of cancer and yet, the patient is rarely, if ever, informed of the associated risks.
Currently, doctors tend to opt for 1 of 3 choices: no mention of risk; understatement of risk or full disclosure of risk.
No mention of risk
Some doctors choose not to mention any risks involved. These may be very real and quite substantial but they remain unsaid and unheard, the main reason being that radiologists are too busy too explain the risks and to get an informed consent. However, the patient’s rights are not just overshadowed by the factor of efficiency but also that of a paternalistic attitude of “doctor knows best”.
Understatement of risk
In nuclear medicine, the standard practice is to obtain a written informed consent. The only problem is that the quality of the information given to the patients is suspect. Doctors tend to give imprecise statements such as, “A nuclear medicine examination is safe, with an irradiation corresponding to a simple radiograph”.
The attitude is to suggest that the examinations are safe and simple. A patient might believe that a simple radiograph would be a chest X-ray, the simplest and commonest radiological examination.
In reality, the dose exposure could be very much higher. While the purpose of such imprecise statements might be to reassure or prevent unnecessary concern about an unavoidable risk, the fact remains that the associated risks are underestimated and the patient’s autonomy is eroded.
Full disclosure
Full disclosure involves informing the patient of any possible risk however small. It also means that the patient has clearly understood the benefits vs the risks involved in the radiological examination or procedure. He then makes an informed choice which means that the consent obtained is an informed one (informed consent). However, only a few doctors, if any, provide full disclosure.
Reasons for the failure to communicate the risks
It must be understood that failure to communicate the risks of radiological and nuclear medicine to patients is violating patient autonomy. There could be various reasons for this failure, but this is no excuse as the risks are real and may be substantial depending on the type of procedure carried out.
Some of the reasons for failing to communicate risks include:
1. The practitioner has a morbid fear of losing his patient if he alarms him. A simple example is to label drugs scheduled as poisons with a poison label. Many doctors opt not to do so as this might scare the patient from consuming the drug. What more if you talk of cancers, leukaemia and death as a result of irradiation!
2. Another factor in carrying out a hazardous procedure without a clear idea of the benefits is the fear that if you don’t carry out that procedure, another doctor would be willing to. The following remark from a senior surgeon that if he didn’t remove the appendix from a patient complaining of abdominal pain, someone else would do it even though the appendix might not be the primary cause of the problem would serve to illustrate this point.
3. The terminology used in radiation protection can be mind-boggling even to doctors and specialist in other fields. Terms like “megabecquerels”, “roentgen”, “millicuries”, “millirems”, “micro-sieverts”, “source-related dose cconstraints” and “co-efficient for stochastic effects” are employed in this branch of medicine which sets standards for the safe use of irradiation. The communication between doctors themselves is lost in this quagmire of gobbledygook. Unfortunately, the end result is that risks get ignored at the expense of the poor patients.
As it is essential to communicate risks to patients, one way out is to simplify the language such that the layman understands it and in so doing will be able to give an informed consent whether he wishes to undergo the procedure or not.
